Urinary Incontinence
Overview
Bladder control problems range from urinating too frequently to actual leakage (urinary incontinence). These problems affect nearly 13 million people of all ages and both sexes in the United States. Approximately 85 percent of those afflicted are women. Unfortunately, many people feel so ashamed that they may even hide their problem from their doctor. If your incontinence interferes with your daily life, seek help promptly. Our experienced urologists can recommend many new treatments to cure or manage your problem, letting you resume a normal life free from worry and shame.
Symptoms
Urinary incontinence is the involuntary loss of urine. It is not a disease but rather a symptom that can be caused by a wide range of conditions. Incontinence can be caused by diabetes, a stroke, multiple sclerosis, Parkinson’s disease, some surgeries or even childbirth. More than 15 million Americans, mostly women, suffer from incontinence. Although it is more common in women over 60, it can occur at any age. Most health-care professionals classify incontinence by its symptoms or circumstances in which it iccurs. In the normal population, the incidence of incontinence in the female over 65 is more than 25 percent and in the male it is about 15 percent.
What are the various types of urinary incontinence?
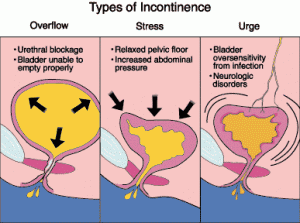
- Stress Urinary Incontinence – Stress urinary incontinence is the most common type of leakage. This occurs when urine is lost during activities such as walking, aerobics or even sneezing and coughing. The added abdominal pressure associated with these events can cause urine to leak. The pelvic floor muscles, which support the bladder and urethra, can be weakened, thus preventing the sphincter muscles from working properly. This can also occur if the sphincter muscles themselves are weakened or damaged from previous childbirth or surgical trauma. Menopausal women can also suffer from small amounts of leakage as a result of decreased estrogen levels. In men, the most common cause of incontinence is surgery on the prostate. This is more frequent after radical prostatectomy for cancer than after transurethral surgery for BPH.
- Urge Urinary Incontinence – Also referred to as “overactice bladder,” urge incontinence is another form of leakage. This can happen when a person has an uncontrollable urge to urinate but cannot reach the bathroom in time and has an accident. At other times, running water or cold weather can cause such an event. Some people have no warning and experience leakage just by changing body position (e.g., getting out of bed). Overactive bladder is also associated with strokes, multiple sclerosis and spinal cord injuries.
- Overflow Incontinence – This type of incontinence occurs when the bladder is full, is unable to empty and yet leaks. Frequent small urinations and constant dribbling are symptoms. This is rare in women and more common in men with a history of surgery or prostate problems.
- Mixed Urinary Incontinence – Mixed incontinence refers to a combination of types of incontinence, most commonly stress and urge incontinence.
Diagnosis
As with any medical problem, a good history and physical exemination are critical. A urologist will first ask questions about the individual’s habits and fluid intake as well as their family, medical and surgical history. A thorough pelvic examination looking for correctable reasons for leakage, including impacted stool, constipation and hernias will be conducted. Usually a urinalysis and cough stress tests will be conducted at the first evaluation. If some findings suggest further evaluation, other tests may be recommended — such as a cystoscopy or even urodynamic testing. This outpatient test is usually done with a tiny tube in the bladder inserted through the urethra and sometimes with a small rectal tube as well.
Treatments
Treatment will depend on your type of incontinence and its cause. Thankfully, most people can be treated successfully, allowing them to enjoy a normal life again. Your doctor may start with less invasive treatments first, such as behavioral changes or medication, and then use medical devices or surgery if other treatments don’t adequately address your incontinence. Blockages usually must be treated surgically; however, those caused by prostate enlargement maybe treated with medication.
MEDICATION
Stress incontinence may be treated with drugs that tighten the bladder neck, such as pseudoephedrine or imipramine. Just as pseudoephedrine causes constriction of the blood vessels in the nose, it also causes the muscles at the bladder neck to contract. Because of its effect on the smooth muscle in blood vessels, it should not be used with a history of hypertension. Imipramine is a tricyclic antidepressant. In addition to causing the bladder muscle to relax, it also causes the smooth muscles at the bladder neck to contract. Urge incontinence is also treated with drugs that have anticholinergic properties. Anticholinergics allow for relaxation of the bladder smooth muscle. A commonly used anticholinergic is oxybutynin chloride. This drug works well to treat urge incontinence but has side effects including dry mouth, confusion, constipation, blurred vision and an inability to urinate. New drugs or new formulations of older drugs have been developed in an effort to reduce side effects. Oxybutynin is now formulated in a slow-release tablet taken once daily. The slow release of this new drug allows for a steady level of the drug and fewer side effects.
Tolterodine tartrate is another new anticholinergic that is different than the older ones in that it has less effect on the salivary glands and therefore causes less dry mouth. It is also available in a slow-release, one-a-day form. Postmenopausal women with incontinence may benefit from hormone treatment. Normally the bladder neck and the urethra are closed at rest. With loss of estrogen, the tissues become weakened or dried and normal closure is lost. Hormone replacement improves the health of these tissues and allows for closure to be regained through increased tone and improved blood supply.
MINIMALLY INVASIVE MANAGEMENT
Some of the causes of incontinence are temporary and easily reversible. Reversible causes include urinary tract infection, vaginal infection or irritation, medication, constipation and restricted mobility. However, in some cases, further medical intervention is necessary. Minimally invasive treatment options are those treatments that do not involve surgery and should be the first line of treatment for patients. However, they may also be used in conjunction with surgical therapy.
Fluid Management: this option consists of instructing a patient to increase or reduce their fluid intake. Incontinent patients may need to reduce the amount of caffeine or other dietary irritants (such as acidic fruit juices, colas, coffee and tea), while at the same time increase water intake to produce an adequate amount of non-irritating, non-concentrated urine. A recommended water intake is six to eight glasses per day.
Bladder Training: A diary is the starting point for bladder training. Patients are instructed to record fluid intake, urination times and when their urinary accidents occur. The diary allows the patient to see how often they actually urinate and when incontinence occurs. The diary is also used to set time intervals for urination. Patients who urinate infrequently are instructed to do “timed urination” where they urinate by the clock every one to two hours during waking hours. By achieving regular bladder emptying they should have fewer incontinent episodes. Timed urination may be effective in patients with both urge and stress incontinence.
Bladder Retraining: Bladder retraining is used for patients with urinary frequency. The goal of retraining is to increase the amount of urine that the patient can hold within their bladder. Patients are instructed to keep a diary to determine their urination interval. Patients are then instructed to gradually increase their urination interval by 15 to 30 minutes per week. The goal is to have patients urinating every two to four hours while awake with less urgency and less incontinence.
Pelvic Floor Exercises: Also known as Kegel exercises, this type of minimally invasive treatment focuses on strengthening the external sphincter muscle and the pelvic muscles. Patients who are able to contract and relax their pelvic floor muscles can improve their strength by doing the exercises regularly. Other patients require help from a health-care professional to learn how to contract those muscles. Biofeedback and electrical stimulation can be used to aid patients in doing pelvic floor exercises. During electrical stimulation, a small amount of stimulation from a sensor placed in the vagina or rectum is delivered to the muscles of the pelvic floor. Like any exercise program, the patient must continue to do the exercises to maintain the benefit. Patients with stress incontinence benefit from pelvic floor exercises by increasing resistance at the urethra and by increasing the strength of the voluntary pelvic floor muscles. Patients can also be taught to compensate by contracting the pelvic muscles with certain activities like coughing. Pelvic floor muscle exercises are effective for urge incontinence, since a contraction of the pelvic floor can interrupt a contraction of the bladder smooth muscle and stop or delay an accident.
SURGICAL MANAGEMENT
In most cases of incontinence, minimally invasive management (fluid management, bladder training, pelvic floor exercises and medication) is prescribed. However, if that fails, surgical treatment can be necessary.
Stress Incontinence: One of the surgical treatments for this condition in males is the use of urethral injections of bulking agents to improve the function of the sphincter. The injections are done under local anesthesia and can be repeated. Unfortunately, the cure rate is only 10 to 30 percent. Another alternative is to perform a urethral compression procedure with the use of a vascular graft or a segment of cadaveric tissue to compress the urethra in the area between the scrotum and the rectum. The results are very preliminary and at this time only experimental. The most effective treatment for male incontinence is implantation of an artificial sphincter. The device is inserted under the skin and consists of a cuff around the urethra, a fluid-filled, pressure-regulating balloon in the abdomen and a pump in the scrotum which is controlled by the patient. The fluid in the abdominal balloon is transferred to the urethra cuff, closing the urethra and preventing leakage of urine.
Stress incontinence in the female is treated at the beginning with behavior modification and pelvic exercise. Sometime techniques like biofeedback or electrical stimulation of the pelvic muscles can help. But when the symptoms are more severe and conservative measures are not helping the treatment is surgery. In selected cases bulking agents can be used to increase continence. The operation is done under local anesthesia and is minimally invasive but the cure rates are lower compared to open surgical procedures.
Anterior repair (Kelly plication) is a common option used by gynecologists but has not given good long-term results. Another option is abdominal surgery (Burch suspension) in which the vaginal tissues are affixed to the pubic bone. The long-term results are good but the surgery requires longer recuperation time and is generally only used when other abdominal surgeries are also required. The most common and most popular surgery for stress incontinence is the sling procedure. In this operation a strip of tissue is applied under the urethra to provide compression and improve urethral closure. The operation is minimally invasive and patients recuperate very quickly. The tissue used to create the sling can be a segment of the patient’s abdominal wall, specially treated fascia, skin from a cadaver or a synthetic material.
Urge Incontinence: For urge incontinence there is a large array of treatment options available. The first step should be behavior modification — drinking less fluids; avoiding caffeine, alcohol or spices; not drinking at bedtime and urinating around the clock and not at the last moment. Exercising the pelvic muscle (Kegel exercises) also helps. It is important to keep a log on the frequency or urination, number of accidents, the amount lost, the fluid intake and the number of pads used if required. The mainstay of treatment for overactive bladder is medication. This consists of the use of bladder relaxants that prevent the bladder from contracting without the patient’s permission. The most common side effect of the medication is dryness of the mouth, constipation or changes in vision. Sometimes, reduction of medication takes care of the side effects.
Other alternatives can be considered in patients who fail to respond to behavior modification and/or medication. A new and exciting technology is the use of a bladder pacemaker to control bladder function. This technology consists of a small electrode that is inserted in the patient’s back close to the nerve that controls bladder function. The electrode is connected to a pulse generator and the electrical impulses control bladder function. There is more than 60 to 75 percent cure or improvement with this technology. In more difficult cases, the bladder can be made bigger using a segment of small intestine. This operation, called augmentation cystoplasty, is very successful in curing incontinence, but its main drawback is the need in 10 to 30 percent of the patients to perform self-catherization to empty their bladder.
Overflow Incontinence: For overflow incontinence, the treatment is to completely empty the bladder and prevent urine leakage. Patients with diabetic bladder or patients with prostatic obstruction often develop this type of incontinence. Overflow incontinence due to obstruction should be treated with medication or surgery to remove the blockage. If no blockage is found, the best treatment is to instruct the patient to perform self-catherization a few times a day. By emptying the bladder regularly the incontinence disappears and the kidneys are protected.
Lifestyle Changes
- Fluid and diet management – avoid caffeinated or tomato-based food and drink, and drink adequate water
- Bladder retraining – follow a schedule for bathroom trips and gradually increase the length of time between them to improve your bladder control
- Pelvic floor (Kegel) exercises – learn techniques to strengthen your pelvic muscles
- Biofeedback – can help you determine when you’re exercising the right muscles
- Special absorbant pads and underwear – these have improved in recent years and can help you feel more confident, especially while undergoing diagnosis and initial treatment