Kidney Cancer
Overview
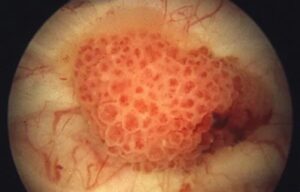
It is important to realize that with timely diagnosis and treatment, kidney cancer can be cured. If found early, the survival rate for patients with kidney cancer ranges from 79 to 100 percent.
The kidneys are two large bean-shaped organs fixed to the upper back wall of the abdominal cavity. One kidney is just to the left and the other just to the right of the backbone. Both are protected by the lower ribcage.
The kidneys main function is to filter the blood and rid the body of excess water, salt, and waste products. The filtered waste products are concentrated into urine. Urine leaves the kidneys through long slender tubes called ureters that connect to the bladder. Urine flows down the ureters into the bladder where it is stored until urination. The kidney also manufactures a hormone called erythropoietin that stimulates the production of red blood cells.
When the kidneys are damaged or a significant portion of kidney tissue is removed, the normal processes listed above may be impaired. In most cases, mild to moderate impairment causes very minor problems. In cases when kidney function is severely impaired, dialysis may be required.
Symptoms
Many kidney tumors do not produce symptoms, but may be detected incidentally during the evaluation of an unrelated problem. Compression, stretching and invasion of structures near the kidney may cause pain (in the flank, abdomen or back), palpable mass, and blood in the urine (microscopic or grossly visible). If cancer spreads (metastasizes) beyond the kidney, symptoms depend upon the involved organ. Shortness of breath or coughing up blood may occur when cancer is in the lung, bone pain or fracture may occur when cancer is in the bone and neurologic symptoms may occur when cancer is in the brain. In some cases, the cancer causes associated clinical or laboratory abnormalities called paraneoplastic syndromes. These syndromes are observed in approximately 30 percent of patients with kidney cancer and can occur in any stage (including cancers confined to the kidney). Symptoms from paraneoplastic syndromes include weight loss, loss of appetite, fever, sweats and high blood pressure. Laboratory findings include elevated red blood cell sedimentation rate, low blood count (anemia), high calcium level in the blood, abnormal liver function tests, elevated alkaline phosphatase in the blood, and high blood count. In many cases, the paraneoplastic syndrome resolves after the cancer is removed.
Diagnosis
Unfortunately, there are no blood or urine tests that directly detect the presence of kidney tumors.
When a kidney tumor is suspected, a kidney imaging study is obtained. The initial imaging study is usually an ultrasound or CT scan. In some cases, a combination of imaging studies may be required to completely evaluate the tumor. If cancer is suspected, the patient should be evaluated to see if the cancer has spread beyond the kidney (metastasis). An evaluation for metastasis includes an abdominal CT scan or MRI, chest X-ray and blood tests. A bone scan is also recommended if the patient has bone pain, recent bone fractures, or certain abnormalities on their blood tests.
Treatments
When the tumor appears confined to the kidney ( a “localized” tumor), there are three main treatment options; tumor removal, tumor ablation and surveillance. Chemotherapy, hormone therapy and radiation therapy are not effective treatments for kidney cancer.
TUMOR REMOVAL
Tumor removal is considered the standard mode of therapy for most patients and is accomplished by performing a surgery called nephrectomy. Radical nephrectomy is surgical removal of everything within Gerota’s fascia, including the whole kidney. Partial nephrectomy is surgical removal of part of the kidney (in this case, the part that contains the tumor). The goal of partial nephrectomy is to remove the entire tumor while preserving as much normal kidney tissue as possible. The kidney tissue that is conserved may prevent the need for dialysis if subsequent kidney damage occurs. Nephrectomy can be performed through a traditional incision (open surgery) or through several small incisions (laparoscopic or retroperitoneoscopic surgery).
TUMOR ABLATION
Tumor ablation destroys the tumor without removing it. Examples of ablative technologies include cryotherapy, interstitial radiofrequency ablation, high-intensity focused ultrasound, microwave thermotherapy and laser coagulation. Ablation can be accomplished during open surgery, laparoscopy, retroperitoneoscopy or percutaneously (through the skin). Since renal tumor ablation is a relatively new procedure, long-term results are unknown. However, ablation may be less invasive than nephrectomy and may be useful in patients who cannot tolerate a more extensive surgery. Tumor ablation may also permit a better chance of preserving kidney function in situations when multiple tumors are present.
SURVEILLANCE
Surveillance may be appropriate when any of the following are present: the kidney tumor has a low probability of being cancer; the patient cannot tolerate treatment; the patient has a short life expectancy (i.e., they are likely to pass away from other causes); or the patient does not want treatment. With lesions that have a low probability of being cancer, regular follow up with a physician is mandatory.
Risk Factors
The following associations may increase the risk of developing kidney cancer:
- Smoking
- Family history of kidney cancer
- Polycystic kidney disease
- Chronic kidney failure and/or dialysis
- Diet with high caloric intake or fried/sauteed meat
- Low vitamin E intake
- Diuretic use or hypertension, although this is still somewhat controversial
- von Hippel Lindau disease
- Tuberous sclerosis
- Exposure to asbestos, blast furnaces and ovens used in iron/steel manufacturing