High BMI and Kidney Transplant Waitlisting
Overweight is defined as having a body mass index (BMI) of 25 to 30 kg/m2, and obesity is a BMI above 30 kg/m2. A BMI above 35 or 40 kg/m2 is considered “morbid obesity.” If dialysis patients are labeled as morbidly obese based on BMI, they they may not be allowed to be actively waitlisted for kidney transplantation according to most, but not all, transplant programs. Hence, many obese dialysis patients are asked to lose weight to qualify for kidney transplantation. If such usual weight reduction programs as dieting or anti-appetite medications do not work, some patients will be introduced to more aggressive interventions such as bariatric surgery.
Obesity Paradox
Overweight and obesity have become mass phenomena with a pronounced upward trend in both developed and developing countries alike. In the general population, obesity is associated with an increased risk of metabolic syndrome, type 2 diabetes, and cardiovascular disease. However, in dialysis patients, an “obesity paradox” whereby a high BMI is incrementally associated with greater survival has been reported consistently. Indeed, dialysis patients who lose weight have increased death risk, whereas those whose dry weight increases live longer. Hence, not only higher BMI but also gaining edema-free weight appears to offer survival advantages to dialysis patients. Recent data suggest that this seemingly paradoxical phenomenon is also observed in dialysis patients who are transplant waitlisted.
Beyond BMI
BMI cannot differentiate between adiposity and muscle mass and, therefore, may not be an acceptable metric with which to assess the body composition of dialysis or transplanted patients. More accurate and differential assessment of lean body mass, in particular, skeletal muscle, and fat mass are needed before attributing high BMI to obesity. Nevertheless, at the population level, most individuals with high BMI are likely to be truly obese people, and this proportion is presumably even higher among dialysis patients, who are inherently multi-morbid with less physical or athletic activities.
There are more elaborate approaches than BMI to assess body composition, such as imaging techniques. A computed tomography and magnetic resonance imaging scan of even a portion of the body (such as abdomen) can be used to estimate total body fat and muscle mass. Bio-electric impedance analysis (BIA) is another method used increasingly in conjunction with regular weight scales, although fluid status instability in a dialysis patient may confound the accuracy of BIA-based estimates of body composition.
Alternatively, recent studies have revived the use of inexpensive and routinely measured surrogate markers such as serum creatinine, waist and hip circumference or mid-arm muscle circumference. Among biochemical markers of muscle mass, serum creatinine is most routinely measured, but its association with kidney function has hampered its utility as such.1 Nevertheless, in long-term dialysis patients with minimal or no residual renal function who undergo a stable dialysis treatment regimen, time-averaged serum creatinine concentration appears to be a more likely surrogate of muscle mass, and its changes over time may represent parallel changes in skeletal muscle mass.2,3
Survival in waitlisted patients
Kidney transplantation is the treatment of choice in patients with end-stage renal disease because patients with functioning kidney allografts have both survival benefits and better quality of life compared with transplant-waitlisted patients on maintenance dialysis. Approximately 80,000 (about 18%) of the 450,000 U.S. dialysis patients are currently on transplant waiting lists, although each year only about 17,000 of these patients receive a kidney transplant. Half of these patients receive a deceased or cadaver kidney, which currently requires a wait period of three to seven years based on the region and state.4 During this period, up to 40% of the transplant-waitlisted dialysis patients die.5
Overweight and obesity are highly prevalent in patients at the time of kidney transplantation. Many transplant centers may suspend waitlisting of obese patients with a BMI above 35 kg/m2 and refer them for weight reduction procedures such as bariatric surgery as a contingency for the transplant surgery.6 In a recent report, a BMI of 35 kg/m2 or higher was the third most common reason to deny patient active transplant-waitlisting, affecting approximately 10% of potential renal transplant candidates.7 However, consequences of obesity or changes in weight during the years of waitlisting remain unclear. Weight changes prior to transplantation may be transient, especially because most renal transplant recipients experience weight gain following a successful kidney transplant,8 Hence, weight loss before transplantation might not alleviate the risk of obesity after transplantation.
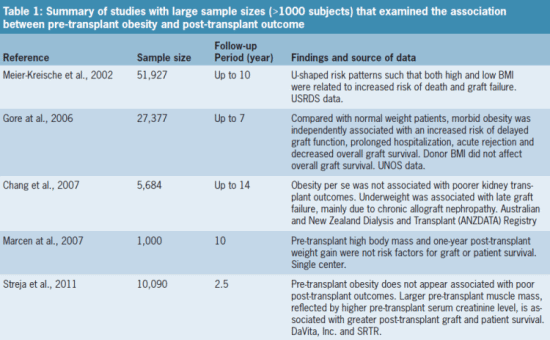
Several studies have examined the issue of obesity in renal transplantation (Table 1). In a recent six-year (2001-2007) cohort study of a national database of a large dialysis organization, the outcomes of 14,632 waitlisted hemodialysis patients without kidney transplantation were examined.9 Low BMI and low serum creatinine—as a surrogate of muscle mass—and their decrease over time were associated with an increased death risk. Researchers observed a 20% higher death risk among patients losing more than 5 kg of dry weight compared with patients who had stable weight over time. Compared with the lowest serum creatinine quintile, the fourth and fifth quintiles had 25% and 43% improved likelihood of survival.
Conclusion
Whereas overweight and obesity are highly prevalent and often associated with increased cardiovascular risk and poor survival in the general population, higher BMI or gaining dry weight appear to confer survival advantage.to dialysis patients. The effect of pre- and post-transplant obesity in kidney transplanted patients on long-term allograft and patient survival appears to be more complicated. BMI is unable to differentiate accurately between adiposity and muscle mass in these patients. Assessing lean body mass, in particular skeletal muscle, and fat mass separately are needed using gold standard techniques such as imaging techniques. Alternatively, inexpensive and routinely measured surrogate markers such as serum creatinine, waist and hip circumference, or mid-arm muscle circumference can be used. As before, we should facilitate and advocate more kidney transplantation including in patients whose BMI is above 35 kg/m2 so all patients can equally benefit from the survival and quality of life advantages.
Kamyar Kalantar-Zadeh, MD, MPH, PhD, is affiliated with the Harold Simmons Center for Chronic Disease Research & Epidemiology, Los Angeles Biomedical Research Institute, Harbor-UCLA Medical Center, Torrance, Calif. He also is the Renal & Urology News medical director for nephrology